BETTER MEDICINE AI: HOW MACHINES ARE LEARNING TO SPOT CANCER EARLIER
As cancer cases rise worldwide, one European startup is using artificial intelligence to help doctors detect the disease earlier and work faster. The goal isn’t to replace clinicians, but to give them better tools when time matters most.
“Time is money” in the working world. For a cancer patient, time is life. And for a radiologist, time can be the difference between life and death, between finding a disease quickly, accurately, and then devoting the remaining time to designing the best treatment regimen for the patient.
Cancer is described as a disease of bad luck and bad timing. Cells mutate, tumours grow silently, and by the time symptoms appear, the window for effective treatment is already narrowing. Early detection saves lives, but in practice is constrained by something far more mundane than biology: time.
“The whole purpose is to create intelligent tools for doctors so they can provide better care for their cancer patients,” says Priit Salumaa, co-founder and CEO of Better Medicine.
“Cancer should be detected as early as possible, but a lot of doctors’ time today is spent on manual and repetitive tasks that should be automated.”
Priit’s team used specialised EU funding from the European Innovation Council (EIC) to found the Better Medicine Artificial Intelligence (BMAI) project in late 2023, to develop AI solutions to automate key aspects of cancer diagnosis and tracking – including full-body cancer detection- to reduce radiologists’ workloads significantly.
The project wrapped up in December 2025 with a successful spin-out company – Better Medicine – raising more seed funding on the back of successful research that used now clinically validated AI models to detect and measure cancer-related biology in real patient CT scans.
Its flagship product, BMVision Kidney, was reported in a Nature article in November 2025 as the first CE-certified AI tool for kidney cancer detection under the EU Medical Device Regulation (MDR 2017/745). In clinical use, it has a standalone detection rate of 96% – up to a 99.2% detection rate when paired with a radiologist’s review – and delivered up to 33–52% time savings.
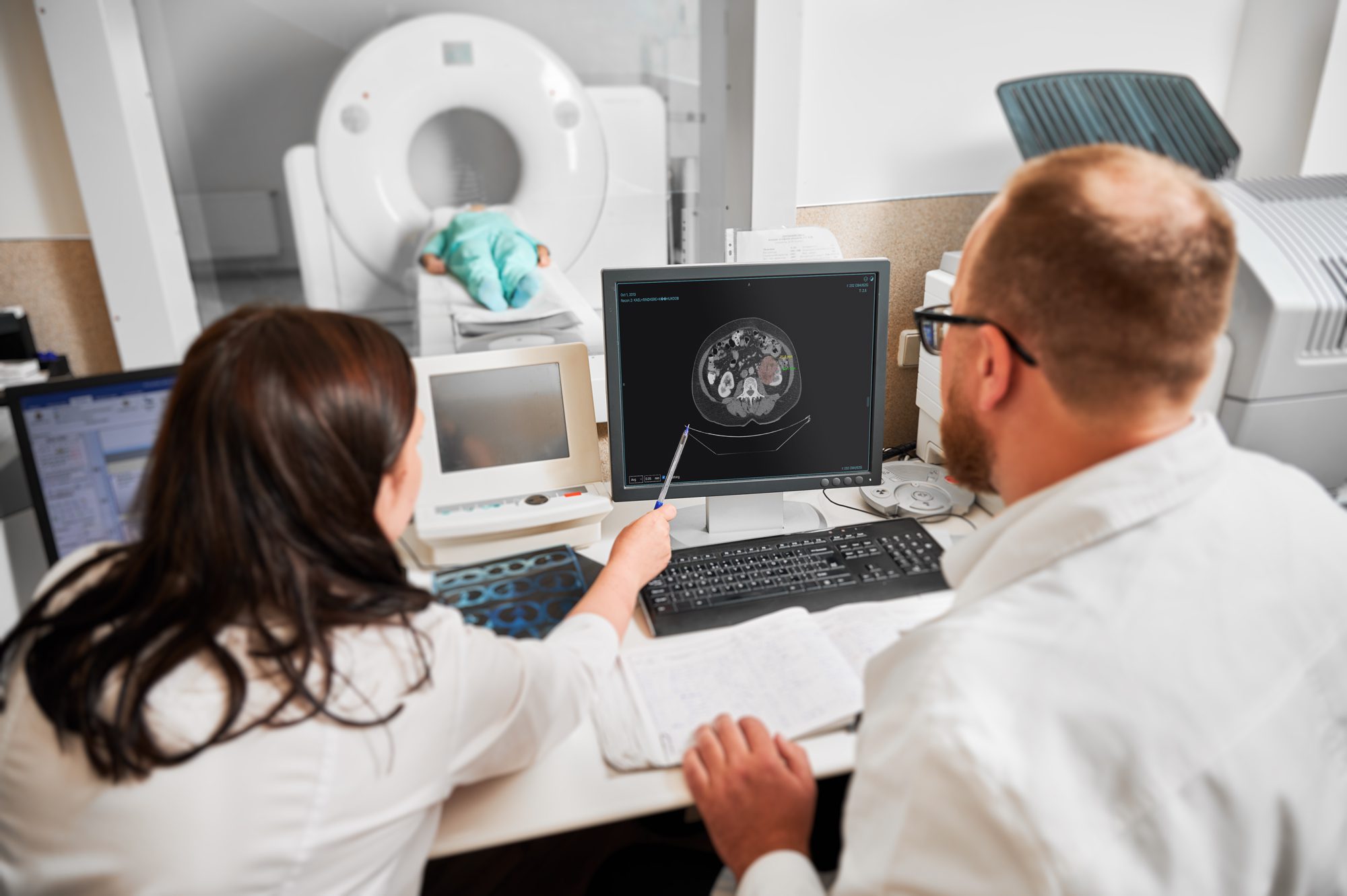
Tick tock tumours
Every family has at least a cancer story. Cancer is the second leading cause of death worldwide (after cardiovascular disease), and in Europe is a significant public health challenge. Europe has only 9% of the global population, but sees 20.3% of cancer-related deaths and 23.4% of diagnoses. Approximately 2.74 million cases were reported in 2022, and are predicted to rise to 3.24 million each year by 2040. Put simply, it is a problem that is getting worse, despite the billions spent on prevention and treatment each year.
CT scans, MRIs and ultrasounds generate huge volumes of visual data, yet radiologists must still examine images slice by slice, annotate findings, compare scans taken months or years apart, and document results with care. It takes years of training. The work is essential, but it is also repetitive, cognitively demanding, and fatigue can lead to mistakes and misdiagnoses.
AI systems trained on medical images offer a way to help. Rather than replacing clinicians, these systems are designed to support them by flagging suspicious regions, prioritising cases that need urgent attention, and automating parts of the reporting workflow. “We scale healthcare capacity through technology, not humans and repetitive work,” Priit says.
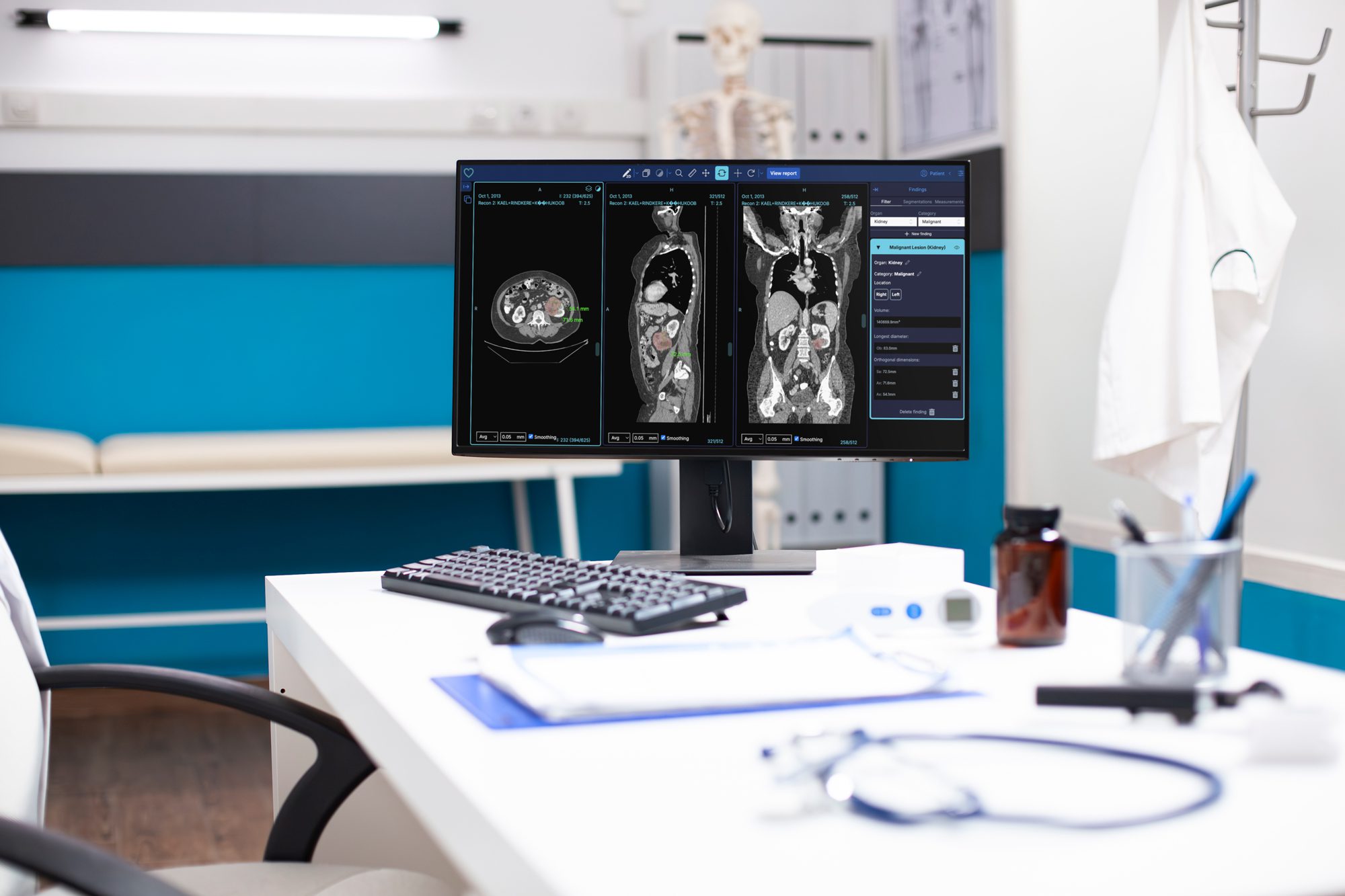
Ironically, radiology is already one of the most digitalised areas of medicine, but Priit says many tools clinicians use are outdated. “Some of the software doctors work with today is like Windows XP,” Priit says. “If you compare that to an iPhone or an iPad, you’re looking at completely different worlds.”
Priit’s background is in computer science and entrepreneurship, not medicine, so he says entering the healthcare world was changing industries completely and a big jump into the unknown. The catalyst came during a routine shoulder operation. “Waking up from the anaesthesia, I had this very clear thought: if you want to do something positive in the world, you should go and study to become a doctor,” he recalls.
The idea did not last long. “When I was fully awake, I realised this was a crazy idea. I was 40 years old. That would take ten years.”
But the broader impulse to make a positive impact stayed with him. During the COVID-19 pandemic lockdowns, Priit used 20 years of experience in product engineering to help organise online hackathons focused on crisis response, bringing together technologists to build digital tools under pressure. “That’s when it really hit me,” he says. “Medicine as an industry is super under-digitalised.” Compared with other sectors, healthcare had been slow to adopt modern software practices, even as data volumes exploded.
Working the problem
From a technological standpoint, AI is well-suited to medical challenges, especially interpreting data from fellow machines. Machine Learning algorithms can process large datasets consistently, identify subtle patterns in the pixels of images, and operate day and night without rest.
But translating that potential into clinical reality is slow. An EIC Accelerator grant is just what Priit needed to transform working prototype modes to a higher Technology Readiness Level. It allowed the BMAI project to focus on innovations in deep learning in medical image analysis, as well as integrating the software with the leading and most commonly used medical platforms.
For an entrepreneur with a background in Software Systems Engineering, nothing can move fast enough. “Everything in medicine takes four to eight times longer than in non-regulated industries,” Priit says. “What could take six to twelve months elsewhere took us four years to certify,” he says.
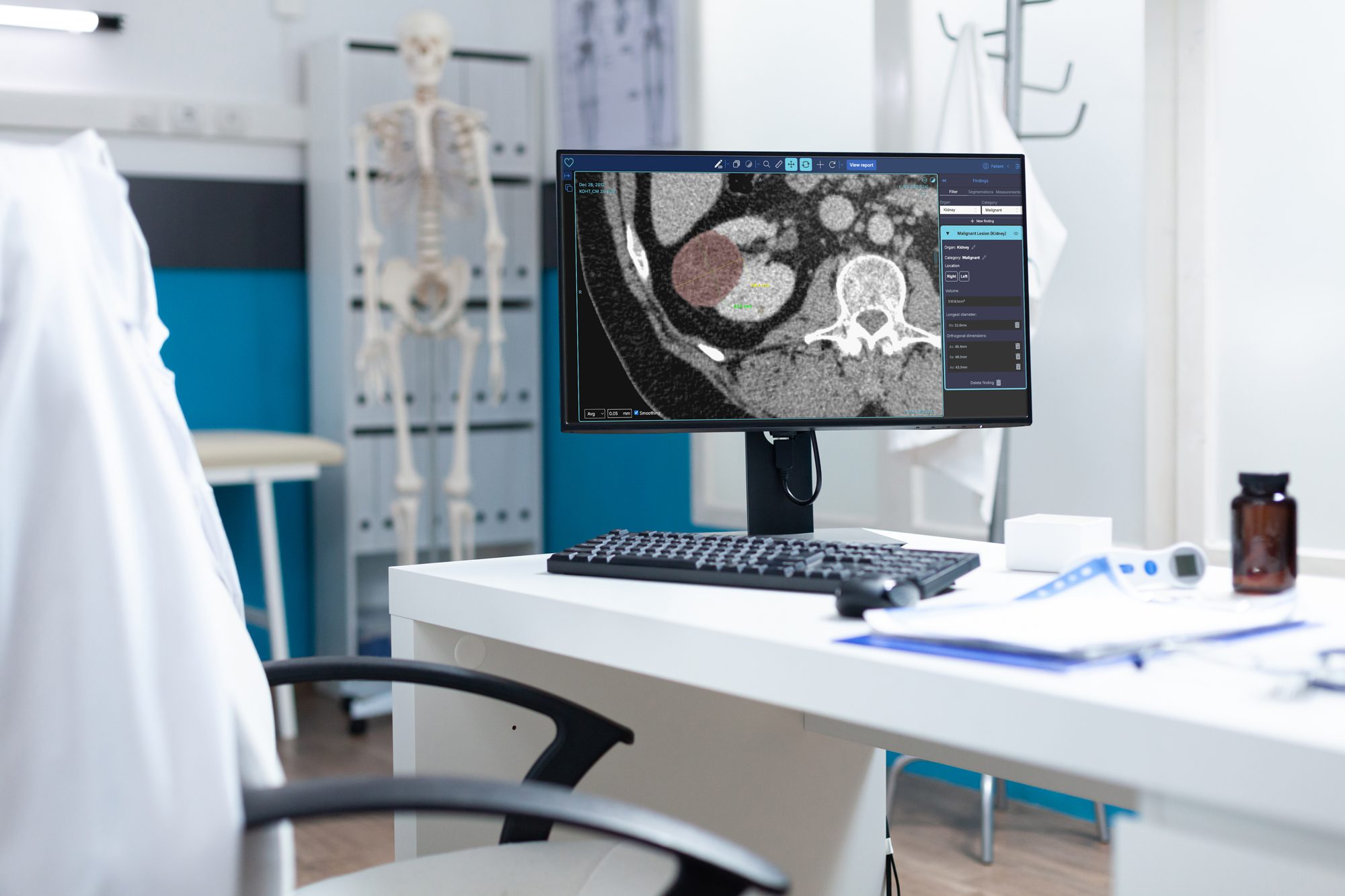
But the certification is necessary, especially in a field where some feel uncomfortable about a machine making a potentially life-or-death diagnosis. Medical AI systems must undergo rigorous clinical validation and meet strict regulatory requirements before they can be used in practice. In Europe, this includes CE certification as a medical device: ‘Conformité Européenne’ marking indicates a product’s compliance with EU safety, health and environmental protection requirements, allowing it to be sold throughout the European Economic Area.
However, regulation also brings trust from the medical and investor communities, with funding from venture capitalists like Soulmates Ventures and angel investors now totalling almost €6 million. “The certification puts a quality stamp on the product,” Priit says. “It tells doctors that this system has been audited from one end to the other.”
Now, the Better Medicine team is distributed across six countries and has secured clinical collaborations with partners including Leeds Teaching Hospitals NHS Trust, Tartu University Hospital, Tartu University, and Pärnu Hospital, amongst others. Priit says the mission itself has been a powerful recruitment tool:
“Saving lives is a much more powerful motivation than building another app.”
The ambition of the research extends beyond the single BMVision Kidney application. The long-term goal is to build AI systems capable of detecting multiple cancers across the body, supporting doctors with consistent, high-quality analysis. “AI is not a silver bullet,” Priit says. “But if it helps doctors work faster, more smoothly, and see things earlier, that can change outcomes for the better.”

Photos by BMAI project
Photo by National Cancer Institute on Unsplash
